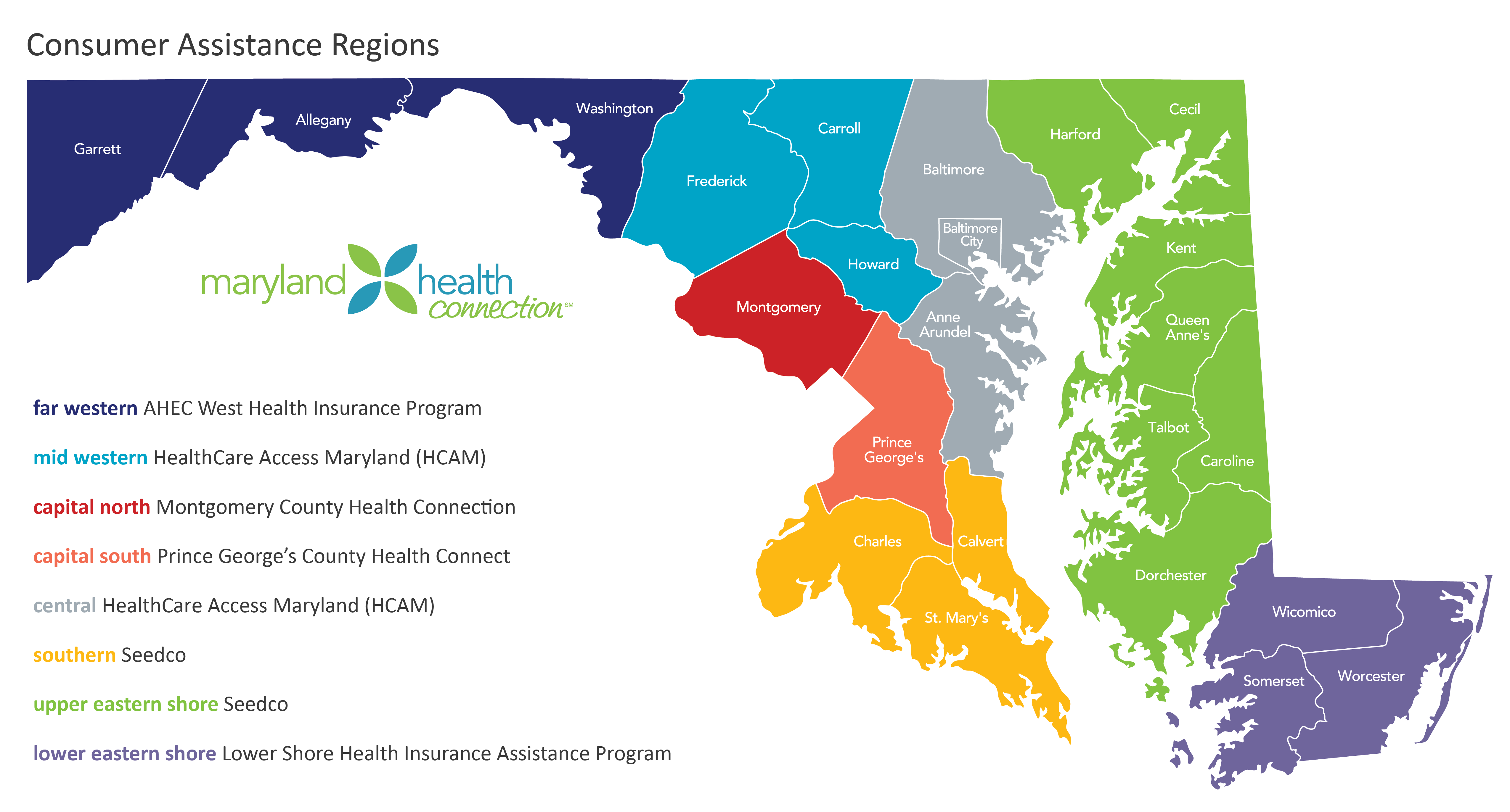
The Connector Program provides free in-person assistance with health coverage, education, eligibility and enrollment for Marylanders. Consumer assistance organizations in eight regions are staffed by trained navigators to help consumers learn about, apply for and enroll in health coverage.
Download Connector Entity Contact Sheet as PDF.
Central Region: Anne Arundel, Baltimore City, Baltimore
Far Western Region: Washington, Allegany, Garrett
Lower Eastern Shore Region: Somerset, Wicomico, Worcester
Mid-Western Region: Howard, Carroll, Frederick
Montgomery County
Prince George’s County
Southern Region: Calvert, Charles, St. Mary’s
Upper Eastern Shore Region: Caroline, Cecil, Dorchester, Harford, Kent, Queen Anne’s, Talbot
For more information contact:
Trina Middleton
Connector Program Manager
trina.middleton1@maryland.gov
National Human Trafficking Hotline
Call (888) 373-7888 Text: 233733
Report fraud, waste or abuse in state government here.
2023 © Maryland Health Benefit Exchange

All rights reserved.
Register to receive updates
National Human Trafficking Hotline
Call (888) 373-7888 Text: 233733
Report fraud, waste or abuse in state government here.

2021 © Maryland Health Benefit Exchange
All rights reserved. Privacy Policy